Case Author(s): Brock G. McDaniel, M.D. and Tom R. Miller, M.D., Ph.D. , 09/04/02 . Rating: #D3, #Q3
Diagnosis: Incompletely obstructing left pulmonary artery embolus.
Brief history:
52 year old woman with two week history of shortness of breath and chest pain.
Images:
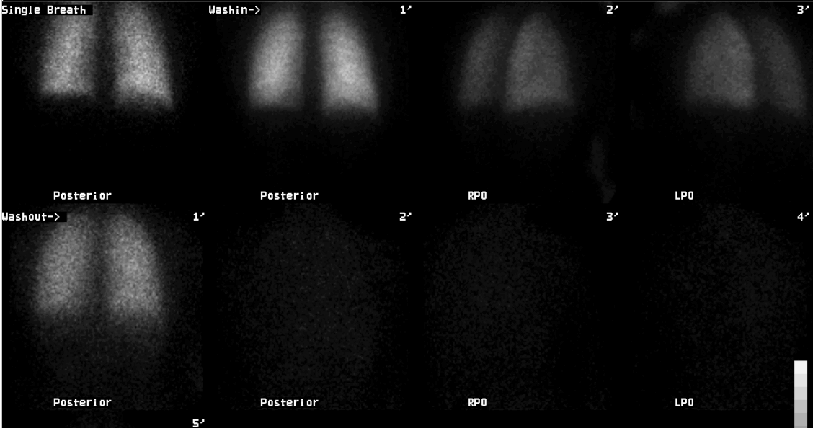
Xenon ventilation
View main image(vq) in a separate image viewer
View second image(vq).
Perfusion
View third image(xr).
Two-view chest radiograph
View fourth image(ct).
Pulmonary emboli protocol CT ( Animated GIF File)
Full history/Diagnosis is available below
Diagnosis: Incompletely obstructing left pulmonary artery embolus.
Full history:
52 year old female with right lower extremity deep venous thrombosis by Doppler ultrasound and elevated D-dimer who presented with a 2 week history of shortness of breath and chest pain.
Radiopharmaceutical:
20.6 mCi Xe-133 gas by inhalation and 4.1 mCi Tc-99m MAA i.v.
Findings:
The ventilation images are normal on single breath, washin and washout phases. There is diffusely heterogeneous perfusion with no segmental perfusion defects. However, there is overall decreased perfusion to the left lung. The PA and lateral chest radiographs were interpreted as normal. The PE-protocol CT demonstrates a large incompletely obstructing pulmonary embolus at the bifurcation of the left main pulmonary artery with involvement of all lobes of the left lung. A smaller right middle lobe embolus is also identified by CT (see animated GIF file).
Discussion:
Classically, findings indicative of a pulmonary embolus include partial or complete absence of perfusion in a segmental distribution in regions of normal ventilation with a normal chest radiograph. This case illustrates an important limitation one must consider when there is relative decreased perfusion to either a segment of lung or an entire lung distribution. In this case, there is a large centrally located clot, which is decreasing the relative flow to the left lung but does not completely occlude it. This can be seen with an incompletely occluding acute pulmonary embolus or during the evolution of a clot with partial recanalization.
Major teaching point(s):
A unilateral perfusion defect is a rare finding. In this case there is also diffusely heterogenous perfusion accompanying the unilateral hypoperfusion. When a unilateral perfusion defect is present with otherwise normal perfusion, the differential diagnosis will depend upon whether there is normal ventilation. With normal ventilation, one should consider disorders such as, fibrosing mediastinitis (Histoplasmosis mediastinitis), mediastinal adenopathy, and less commonly unilateral pulmonary embolus and primary pulmonary artery neoplasms. If the ventilation is absent or decreased, airway obstructive lesions, such as endobronchial adenomas/carcinoid, foreign bodies, mucous plugs and hyperlucent lung syndrome (Swyer-James syndrome) should be considered. With airway obstruction, there is a reflex sympathetic increase in vascular tone thereby decreasing the pulmonary arterial flow to the affected segment/lobe.
Differential Diagnosis List
DDx: Unilateral pulmonary embolus, fibrosing mediastinitis, mediastinal mass/adenopathy, and very rarely primary pulmonary artery neoplasms, such as angiosarcoma.
ACR Codes and Keywords:
References and General Discussion of Ventilation Perfusion Scintigraphy (Anatomic field:Lung, Mediastinum, and Pleura, Category:Other generalized systemic disorder)
Search for similar cases.
Edit this case
Add comments about this case
Return to the Teaching File home page.
Case number: vq048
Copyright by Wash U MO

