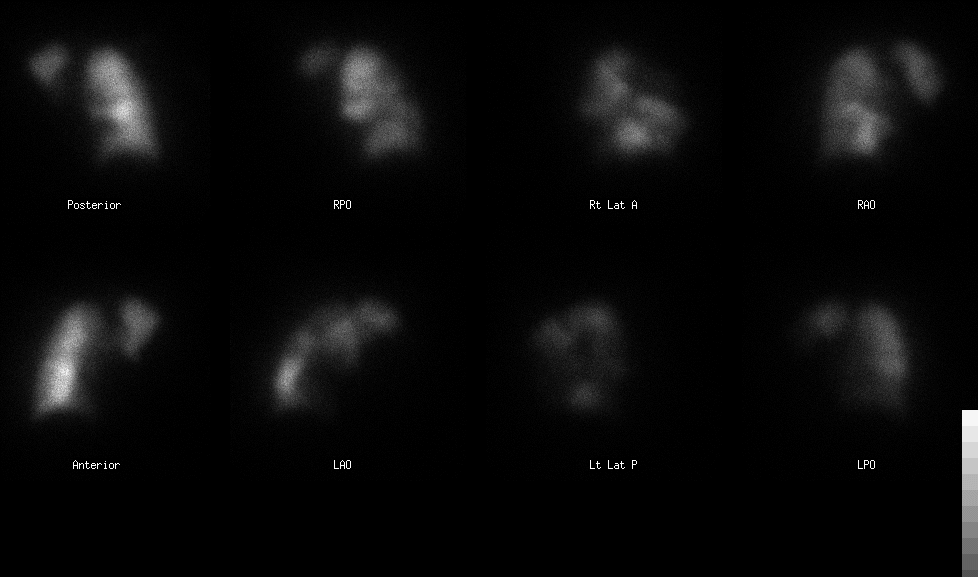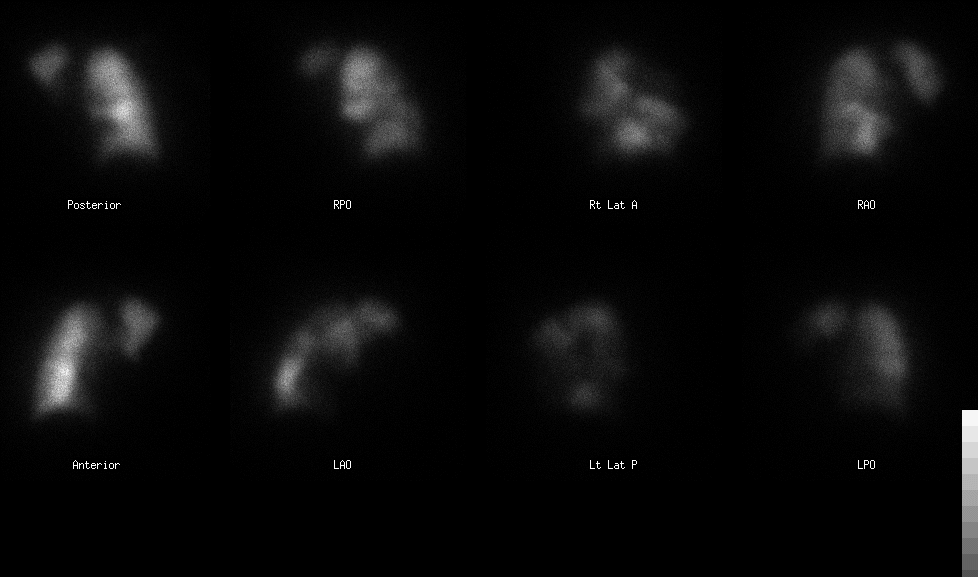Case Author(s): Yonglin Pu, M.D.,Ph.D., Tom R. Miller, M.D., Ph.D. , 11/14/2001 . Rating: #D1, #Q3
Diagnosis: Pulmonary embolism
Brief history:
75 year-old woman with progessive dyspnea.
Images:
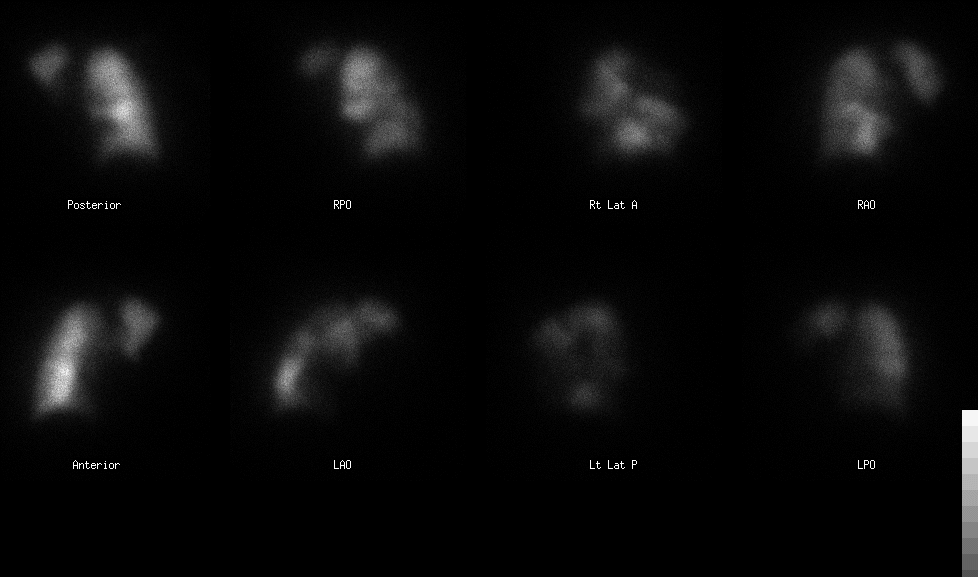
Pulmonary perfusion scintigraphy.
View main image(vq) in a separate image viewer
View second image(vq).
Xenon ventilation scintigraphy.
View third image(ct).
Helical pulmonary CT through hilar and infrahilar regions
View fourth image(xr).
Chest X-ray; frontal and lateral views.
Full history/Diagnosis is available below
Diagnosis: Pulmonary embolism
Full history:
A 75 year-old black female with hypertension, chronic obstructive pulmonary disease, type 2 diabetes, cardiac disstolic dysfunction and obesity came to the emergency room with increasing shortness of breath over five days. She denied chest pain, palpitations, fevers, chills, naussea or vomiting. She did report neck tightness. The troponin was negative. The patient is a smoker and was on Evista, a selected estrogen-receptor modulator.
Radiopharmaceutical:
10.0 mCi Xe-133 gas by inhalation and 3.9 mCi Tc-99m MAA i.v.
Findings:
FINDINGS:
Perfusion Scintigraphy:
The perfusion images show absent perfusion in the entire left lung except the apical posterior segment of the left upper lobe. There is also absence of perfusion in the right posterior basal segment. There is decreased perfusion in the anterior basal segment of the right lower lobe and the anterior segment of the right upper lobe. Ventilation Scintigraphy:
The Xe-133 ventilation images show a uniform distribution of activity on single-breath and washin images. There is minimal abnormal Xe-133 retention in the left lung during the washout phase.
CT was performed the same day as the V/Q study utilizing the pulmonary embolism protocol with i.v. contrast. Extensive acute pulmonary embolism is seen within both lungs. A large clot fills the right main pulmonary artery extending into the right lower lobe and almost including the right lower lobe segmental banches. In addition, clot extends into both the anterior and posterior segmental branches of the right upper lobe. The right middle lobe appears to be free of clot. An even larger thrombus is seen within the main left pulmonary artery,with extensive thrombus occluding all left lower lobe segmental branches. Thrombus extends into lingular branches of the left upper lobe as well as to the proximal left upper lobe anterior branch. There is associated enlargement of the main pulmonary artery with right ventricular enlargement also seen.
Chest radiographs:
No pulmonary infiltrates or pleural effusion.
Discussion:
Pulmonary embolism is a relatively common and potentially fatal disease. The incidence of deep venous thromboembolism (DVT) is approximately one in 1000 per year and about 50% of DVT are complicated with PE. About 10% of patients with PE die within one hour of the PE event. However the treatment for PE with anticoagulants or surgery is highly effective, but it is with complications. Therefore the accurate and prompt diagnosis is very important. The clinical picture of PE is nonspecific, including sudden dyspnea and hypoxemia, pleuritic pain, hemoptysis, substernal pressure, which may mimic coronary artery disease, other kinds of pulmonary diseases, gastroesophageal reflux, plural disease or pericarditis. The risk factors for deep venous thrombosis in lower extremities (DVT) and PE including inactivity/stasis, status post surgery, estrogen use, smoking and hypercoagulable state (1-3).
Comparison of spiral CT and Ventilation-perfusion scintigraphy.
Recently Mayo JR, et al. compared prospectively the accuracy of spiral computed tomography (CT) with that of ventilation-perfusion scintigraphy for diagnosing pulmonary embolism. They performed the study within 48 hours of presentation in 142 patients suspected of having pulmonary embolism underwent spiral CT, scintigraphy, and (when indicated) pulmonary angiography. Pulmonary angiography was attempted if interpretations of spiral CT scans and of scintigrams were discordant or indeterminate and intermediate-probability, respectively. They found that in the 139 patients who completed the study, interpretations of spiral CT scans and of scintigrams were concordant in 103 patients. In 20 patients, intermediate-probability scintigrams were interpreted (six with embolism at angiography, 14 without); diagnosis with spiral CT was correct in 16. Interpretations of spiral CT scans and those of scintigrams were discordant in 12 cases; diagnosis with spiral CT was correct in 11 cases and that with scintigraphy was correct in one. Spiral CT and scintigraphic scans of four patients with embolism did not show embolism. Sensitivities, specificities, and kappa values with spiral CT and scintigraphy were 87%, 95%, and 0.85 and 65%, 94%, and 0.61, respectively. They concluded that in cases of pulmonary embolism, sensitivity of spiral CT is greater than that of scintigraphy. Interobserver agreement is better with spiral CT (4).
Bibliography:
1. Worsley DF and Alavi A. Radionulide imaging of acute pulmonary embolism. Radiologic clinics of North America. 2001;39(5):1035-1052.
2. Dixon AK, Coulden RAR and Peters AM. The non-invasive diagnosis of pulmonary embolus. BMJ 2001;323(25):412-413.
3. Myers A. Pulmonary embolism. In, Myers A edited. Medicine (National medical series for independent study),3rd edition.1997:83-86.
4. Mayo JR, Remy-Jardin M, Muller NL, et al. Pulmonary embolism: prospective comparison of spiral CT with ventilation-perfusion scintigraphy. Radiology. 2001;221:606-613
Followup:
An IVC filter was placed, and the patient was started on coumadin and lovenox.
Major teaching point(s):
This case shows that both Ventilation/Perfusion Scintigrahy and Spiral CT Angiography are both effective in the diagnosis of pulmonary embolisim if emboli are in the central pulmonary arteries.
Differential Diagnosis List
(1) Pulmonary leimyosarcoma.
(2) Centally obstructing mass
(3) Sarcoidosis
(4) Fibrosing Mediastinitis
(5) Radiation Changes
ACR Codes and Keywords:
References and General Discussion of Ventilation Perfusion Scintigraphy (Anatomic field:Lung, Mediastinum, and Pleura, Category:Organ specific)
Search for similar cases.
Edit this case
Add comments about this case
Return to the Teaching File home page.
Case number: vq047
Copyright by Wash U MO