Case Author(s): Lester Johnson, M.D., Ph.D. and Jerold Wallis, M.D. , 1/14/00 . Rating: #D2, #Q4
Diagnosis: Asymmetric chronic obstructive pulmonary disease
Brief history:
Episodic shortness of breath increasing in frequency and severity
Images:
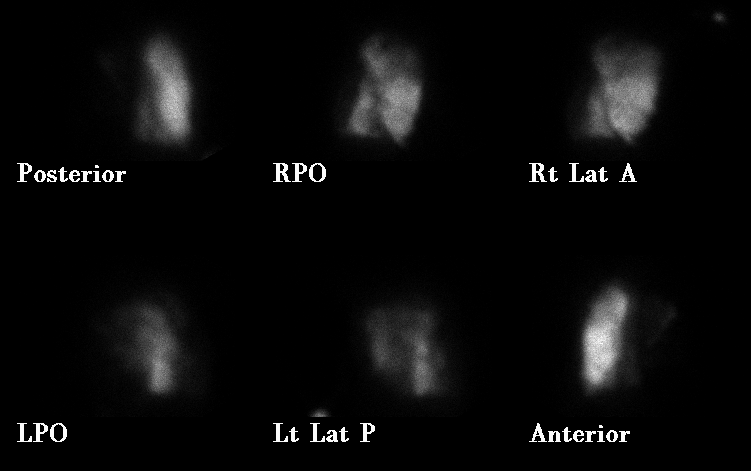
Perfusion
View main image(vq) in a separate image viewer
View second image(vq).
Ventilation
View third image(xr).
A PA radiograph of the chest is shown
View fourth image(xr).
A lateral radiograph of the chest is shown
Full history/Diagnosis is available below
Diagnosis: Asymmetric chronic obstructive pulmonary disease
Full history:
This 64-year-old male smoker has a history of severe chronic obstructive pulmonary disease (COPD). Recently his episodes of shortness of breath have been increasing in frequency and severity. Lower extremity Dopplers were negative for evidence of deep venous thrombosis. This examination was performed to assess and quantitate regional pulmonary function prior to possible surgical intervention such as lung transplantation or lung volume reduction.
Radiopharmaceutical:
Xe-133 gas by inhalation and Tc-99m macroaggregated albumin (MAA) by intravenous injection
Findings:
The Xe-133 washin images show a uniform distribution of activity within the right lung, but almost no activity within the left lung. There is bilateral abnormal Xe-133 retention during the washout phase. The perfusion images demonstrate near total absence of perfusion to the left lung. Perfusion of the right lung is heterogeneous, most preserved in the middle lobe. Based on the distribution of Xe-133 during the early washin phase, the right lung contributes 94% and the left lung 6% of total pulmonary ventilation. The right lung receives 97% and the left lung receives 3% of total pulmonary perfusion. The correlative chest radiograph demonstrates advanced bullous pulmonary emphysema, most severe in the left lower lobe which is virtually replaced by bullae.
Discussion:
While there is a tendency for the findings of chronic obstructive pulmonary disease to be bilateral and most pronounced in the upper lung zones, this case demonstrates how variable in distribution the process can be. The near absence of perfusion to one lung is typically associated with a central (i.e., hilar or mediastinal) pathologic process causing mass effect on pulmonary vessels (e.g., lung carcinoma, fibrosing mediastinitis). Pulmonary embolism is much less likely to produce unilaterally decreased perfusion of a lung or lobe. In this case, however, the grossly abnormal ventilation study with pronounced bilateral xenon retention, and the bullous changes on the chest radiographs, indicate the presence of severe COPD that accounts for the abnormal perfusion.
ACR Codes and Keywords:
References and General Discussion of Ventilation Perfusion Scintigraphy (Anatomic field:Lung, Mediastinum, and Pleura, Category:Organ specific)
Search for similar cases.
Edit this case
Add comments about this case
Return to the Teaching File home page.
Case number: vq042
Copyright by Wash U MO

