Case Author(s): Matt Jaksha, M.D. and Barry A. Siegel, M.D. , 07/18/98 . Rating: #D2, #Q3
Diagnosis: Pumonary arterial hypertensive changes with pneumonitis and bronchiolitis
Brief history:
25-year-old woman with progressive dyspnea on exertion
Images:
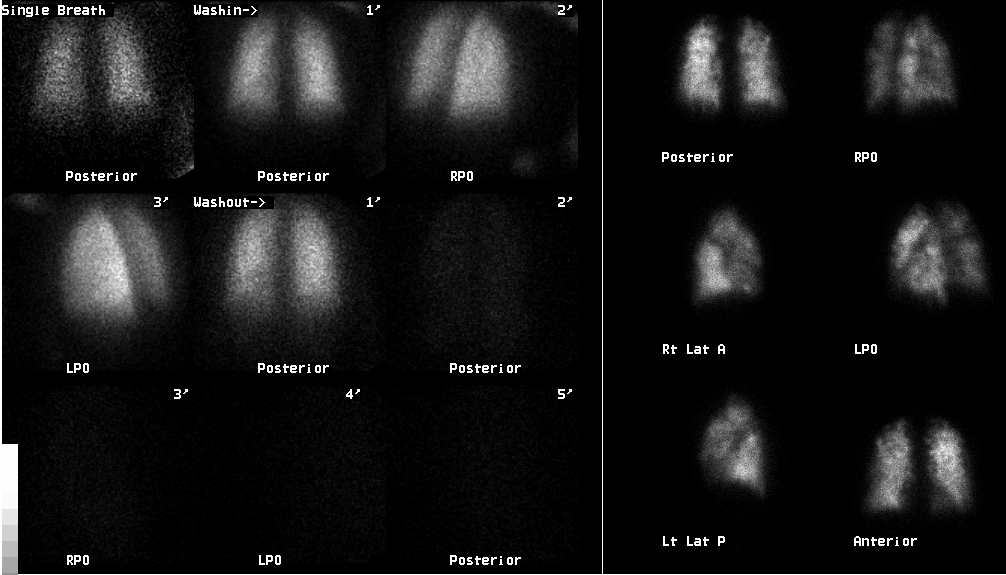
Ventilation and perfusion images
View main image(vq) in a separate image viewer
View second image(xr).
Chest radiograph from the previous day
Full history/Diagnosis is available below
Diagnosis: Pumonary arterial hypertensive changes with pneumonitis and bronchiolitis
Full history:
This is a 25-year-old woman with progressive dyspnea on exertion over two years. During evaluation at an outside hospital, pulmonary hypertension was identified during right heart catheterization. A chest CT demonstrated patchy ground glass infiltrates. Deep venous thrombosis was identified in the right common femoral vein. Ventilation-perfusion scintigraphy was requested for further evaluation and specifically to rule out pulmonary emboli.
Radiopharmaceutical:
Xe-133 gas by inhalation and Tc-99m macro-aggregated albumin i.v.
Findings:
The ventilation study is within normal limits. The perfusion images are diffusely abnormal, with innumerable small perfusion defects resulting in very heterogeneous perfusion. The chest radiograph demonstrates mild prominence of the pulmonary outflow tract, but no other abnormality.
Discussion:
This perfusion pattern makes major thromboembolic disease unlikely. Small pulmonary emboli, both thrombotic and non-thrombotic, are possible. Vasculitis and microthrombotic pulmonary hypertension are possible etiologies.
Followup:
The patient underwent pulmonary angiography the following day. The pulmonary artery pressure was 80/35 (mean 54) mm Hg on the right and 76/36 (mean 53) mm Hg on the left. There were no intraluminal filling defects or wall irregularities to suggest pulmonary emboli. Patchy parenchymal perfusion, most prominently decreased in the right middle lobe, suggested pathology at the arteriolar or capillary level.
Lung biopsy one day later showed pulmonary arterial hypertensive changes, without evidence of pulmonary emboli. Focal chronic intersitial pneumonitis and chronic bronchiolitis was also seen. The changes were not typical of primary pulmonary hypertension, and collagen vascular disease was suggested as a possible etiology.
View followup image(an).
Image of a right pulmonary arteriogram
Differential Diagnosis List
See vq027
ACR Codes and Keywords:
References and General Discussion of Ventilation Perfusion Scintigraphy (Anatomic field:Lung, Mediastinum, and Pleura, Category:Organ specific)
Search for similar cases.
Edit this case
Add comments about this case
Read comments about this case
Return to the Teaching File home page.
Case number: vq031
Copyright by Wash U MO

