Case Author(s): Matt Jaksha, M.D. and Jerold Wallis, M.D. , . Rating: #D4, #Q4
Diagnosis: Quantum Mottle
Brief history:
Shortness of breath for 1 year. Rule out chronic pulmonary emboli.
Images:
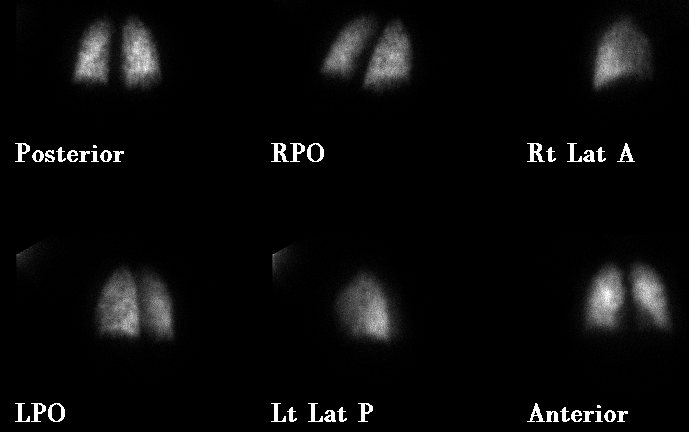
Perfusion images. What is causing the diffuse heterogeneity?
View main image(vq) in a separate image viewer
View second image(vq).
Ventilation images
View third image(xr).
Chest radiograph of the same day
Full history/Diagnosis is available below
Diagnosis: Quantum Mottle
Full history:
This is a 27 year old woman who complains of shortness of breath for
one year. She was initially injected with 4.4 mCi Tc-99m MAA for the
perfusion images of this ventilation-perfusion lung scintigraphy.
Because of the patchy appearance of the study, the technologist was
questioned and reported difficulty with the injection. It took
approximately three times longer than expected to obtain the perfusion
images. Therefore, a second injection was made with an additional
2.8 mCi Tc-99m MAA,
and imaging was repeated.
Radiopharmaceutical:
4.4 mCi and 2.8 mCi Tc-99m macro-aggregated albumin i.v.; 18.2 mCi Xe-133 inhaled gas.
Findings:
The initial perfusion images are patchy, with multiple small perfusion
defects present bilaterally. The ventilation study is normal. The
chest radiograph shows only minimal atelectasis at the right base,
certainly not enough to account for the perfusion abnormality. The
repeat perfusion images (see follow-up image) are normal.
Discussion:
This is an example of image noise due to too few particles, also
referred to as quantum mottle. Poisson statistics affect image
appearance, both in regard to the number of counts (activity) and
the number of particles in a space. While a longer imaging time will
improve counting statistics, it will not affect the distribution of
particles in space. Too few particles in the volume of the lungs can
give a patchy appearance and cause false positive interpretations.
Standardly, 200,000 to 500,000 particles are administered for pulmonary
perfusion scintigraphy. It is generally accepted that administration
of at least 60,000 particles will avoid quantum mottle
(see Statistical Considerations in Lung Imaging with Tc-99m Albumin
Particles, Heck and Duley,Jr., Radiology 1974 Dec;113:675-9). The
number that causes this effect is probably much smaller in the average
patient, but this standard covers variability in lung volume,
respiratory motion, dose left in the syringe, etc.
The problem can result from an error in the radiopharmacy, but more
often results from not enough radiopharmaceutical reaching the patient's
lungs, as in this case. On the initial posterior image, it took 215
seconds to get 467,700 counts. On the repeat posterior image, it took
92 seconds to get 563,898 counts. Assuming that all of the second
injection (2.8 mCi) reached the patient's lungs, we can calculate that
only 1.5 mCi was present initially, or about one third of the
intended 4.4 mCi. This may be tolerated depending on the number of
particles/mCi in the kit. The ratio changes as the kit ages
(radioactivity decreases, while particle number remains the same).
If this occurred near the end of the kit's shelf life, the image may
still have appeared normal, since a larger number of particles would
have been required to give the same tracer dose.
View followup image(vq).
Perfusion images after repeat injection
Differential Diagnosis List
Primary pulmonary hypertension, vasculitis, non-thrombotic emboli
(fat, amniotic fluid, talc, tumor), congestive heart failure have
also been reported to give heterogeneous perfusion
ACR Codes and Keywords:
References and General Discussion of Ventilation Perfusion Scintigraphy (Anatomic field:Lung, Mediastinum, and Pleura, Category:Other(Artifact))
Search for similar cases.
Edit this case
Add comments about this case
Return to the Teaching File home page.
Case number: vq027
Copyright by Wash U MO

