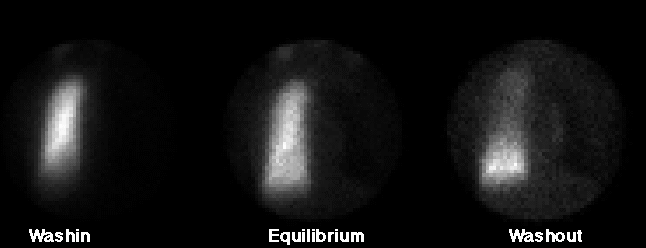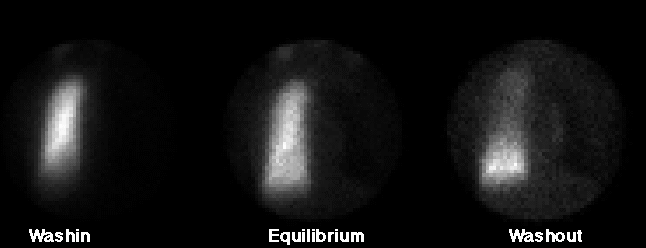Case Author(s): Vreeland, M.D. / Royal M.D. , 11/19/94 . Rating: #D2, #Q5
Diagnosis: Pneumothorax
Brief history:
71 year old man with a right hilar mass
presenting with acute onset of shortness
of breath. Rule out PE.
Images:
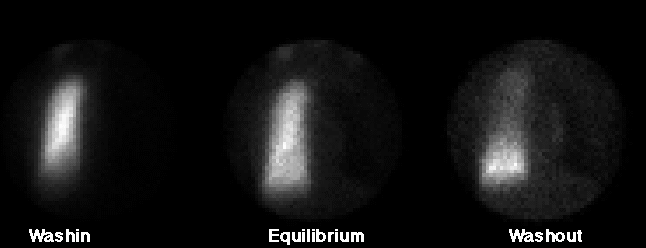
Xenon Ventilation Images
View main image(vq) in a separate image viewer
View second image(vq).
Perfusion Images
View third image(xr).
CXR
Full history/Diagnosis is available below
Diagnosis: Pneumothorax
Full history:
71 year old man with a known right hilar mass presented
with acute worsening of shortness of breath. V/Q scan
was ordered to rule out pulmonary embolism. CXR was
obtained after the scintigraphic evaluation.
Findings:
Ventilation: Xenon-133 ventilation images shows abnormal
ventilation of the left lung, with relative hypoventilation
to the left lung base on washin images, and significant
retention of activity on washout images. Essentially no
activity is appreciated in the right lung on washin images.
Faint activity can be appreciated along the right hilum
on washout images. Upon careful inspection, a photon defecient area encompassing much of the expected area of the right lung, with overall less activity than the normal background is seen.
Perfusion: Perfusion images demonstrate hypoperfusion to
the left lung base in a pattern matching the ventilation
abnormality. In addition, perfusion images demonstrate a
vertical-band of activity extending along the medial aspect
of the right lung on anterior and posterior views. The RPO
view demonstrates the anterior-posterior extent of perfusion
within the right lung. No focal, large, segmental, wedge-shaped
perfusion defects are noted in the left middle and upper lung
fields. Overall, perfusion is slightly better to the right lung
lung, when compared with the same area on the ventilation images.
CXR: Standard chest radiograph obtained after worrysome
findings on the ventilation/perfusion scans demonstrate
a large, secondary pneumothorax, with marked collapse of the
entire right lung.
Discussion:
Unilateral, matching lung defects are unlikely to represent pulmonary
emboli, especially if the other lung is normal or only has
small, peripheral, perfusion defects. Likewise, matching unilateral
lung defects are more likely to be caused by other etiologies.
Secondary pnuemothorax may occur iatrogenically with procedures
or may be secondarily associated with lung or pleural-based
masses, especially in individuals with underlying
cardiopulmonary diseases, such as asthma, COPD, etc.
When evaluating a ventilation/perfusion scan for pulmonary
embolism, one should have a recent, standard chest radiograph.
The chest radiograph should be within 24 hours of the acute
event and prior to performing the V/Q scan. A significant
change in the respiratory status or acute symptoms would
dictate obtaining a more recent chest radiograph, even if a chest
radiograph had already been obtained within 24 hours. A
recent chest radiograph is required to interpret the V/Q scan; however,
more importantly, it may identify other etiologies responsible
for the patient's symptoms, such as pnuemothorax.
Followup:
A chest tube was successfully placed; the patient's symptoms improved
placement of the chest tybe; and, subsequent radiographs
showed reexpansion of the right lung.
Differential Diagnosis List
The most common cause of unilateral lung perfusion
defects result from bronchogenic carcinoma or a space-occupying
lesion. Other less common etiologies include pnuemonectomy,
large pleural effusion, mucous plugging, endobronchial lesion
(iatrogenic), and mediastinal or hilar masses, such as
sarcoidosis, fibrosising mediastinitis, or lymphoma, etc.
uncmommon causes of this finding would include pulmonary
embolisim, Swyer-James Syndrome, foreign body, injection into
a pulmonary catheter, and pulmonary vein or arterial hypoplasia.
ACR Codes and Keywords:
References and General Discussion of Ventilation Perfusion Scintigraphy (Anatomic field:Lung, Mediastinum, and Pleura, Category:Organ specific)
Search for similar cases.
Edit this case
Add comments about this case
Return to the Teaching File home page.
Case number: vq005
Copyright by Wash U MO