Case Author(s): Thomas H. Vreeland, MD / J. Wallis, MD , 7/5/94 . Rating: #D1, #Q4
Diagnosis: Pulmonary Embolism
Brief history:
Progressively SOB, rule out PE
Images:
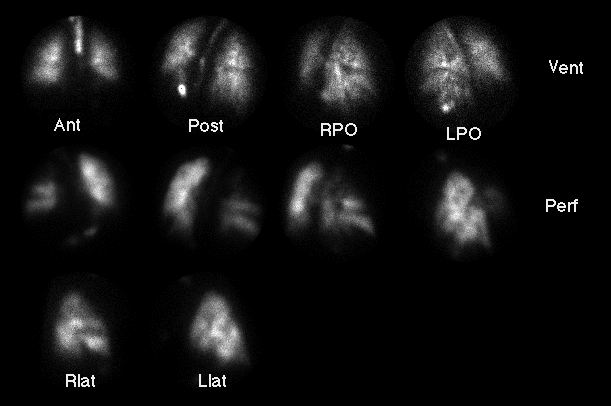
Tc-99m DTPA ventilation images (top) and
Tc-99m MAA perfusion images (below).
View main image(vq) in a separate image viewer
The chest radiograph (not shown) was normal.
Full history/Diagnosis is available below
Diagnosis: Pulmonary Embolism
Full history:
This patient is a 63 year-old man with a history of diabetes
mellitus, who presents with gradual shortness of breath
during the 72 hours prior to admission. The patient had a
widened A-a gradient on two liters of oxygen and,
was subsequently anticoagulated. Ventilation-perfusion
scintigraphy was performed to evaluate for pulmonary embolism.
Findings:
CXR:
No evidence of acute disease. No pleural effusions or
infiltrate identified.
Ventilation Images:
Mild heterogenity of ventilation, with a moderate defect
in the region of the right major fissure.
Perfusion Images: (7/2/94)
Multiple, large, segmental, wedge-shaped, perfusion defects
in both lung fields, with greater involvement of the right
lung than the left lung.
Discussion:
The large perfusion defects noted in both lung fields
without corresponding radiographic or ventilatory
abnormalities present a characteristic scintigraphic
appearance for pulmonary embolism. The results are
best described as yielding a high likelihood
ratio for pulmonary embolism; the test results can
then be combined with the pretest probabilty
for pulmonary embolism to yield the post-test
probability. The
following table illustrates the combination of test
results with the pre-test assessment.
----------------------Posterior probability of PE
Category-----------Li------5%-------15%-------50%-------85%
High------------16.23-----46%-------74%-------94%-------99%
Intermediate-----0.63------3%-------10%-------39%-------78%
Low-------------0.069-----<1%--------1%--------6%-------28%
Followup:
The patient is being treated for pulmonary embolism with
anticoagulation with coumadin.
View followup image(vq).
Although no followup image is availble, this
link shows another example of a high likelihood
study for comparison.
Major teaching point(s):
(1) The bilateral lung involvement with large,
segmental, unmatched
perfusion defects is classic for pulmonary embolism,
and typically negates the need for futher evaluation, i.e.
pulmonary angiography.
(2) It is useful for followup ventilation / perfusion
scintigraphy to be
performed 2 to 4 weeks after the initial study to
establish a new baseline, since a significant number of
perfusion defects will persist for years.
Differential Diagnosis List
(1) Pulmonary Embolism
Other causes of unmatched defects (listed below) would
be unlikely in this case.
(2) Centally obstructing mass
(3) Sarcoidosis
(4) Fibrosing Mediastinitis
(5) Radiation Changes
ACR Codes and Keywords:
References and General Discussion of Ventilation Perfusion Scintigraphy (Anatomic field:Lung, Mediastinum, and Pleura, Category:Organ specific)
Search for similar cases.
Edit this case
Add comments about this case
Return to the Teaching File home page.
Case number: vq001
Copyright by Wash U MO

