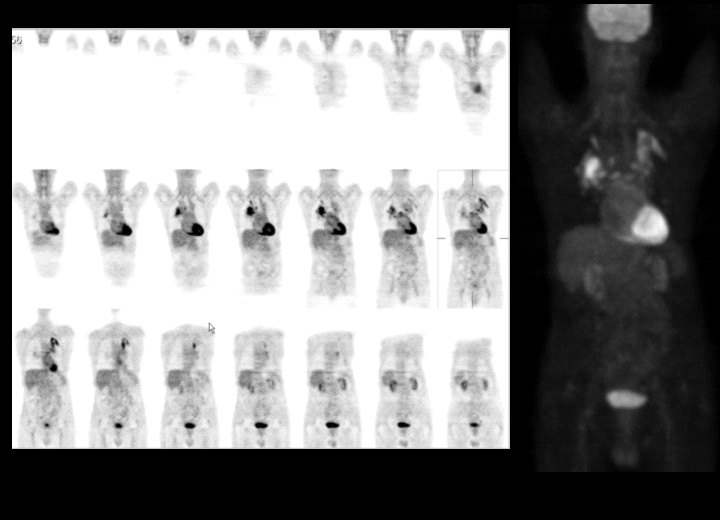

F-18 fluorodeoxyglucose (FDG) imaging of the body.
View main image(pt) in a separate image viewer
View second image(pt). Axial fused FDG-PET and CT Images
View third image(ct). Selected Axial CT Images
Full history/Diagnosis is available below
In the left lung, there is an area of markedly abnormal FDG uptake beginning at the left apex. This abnormality extends down the upper lobe bronchi to involve the left hilum. In addition, this abnormal activity extends down the descending thoracic aorta, and there is a separate continuation adjacent to the oblique fissure. All of these areas of abnormal uptake correspond to soft tissue attenuation in the lung on CT. Mild FDG uptake is noted along with peri-bronchovascular thickening of the left lower lobe bronchi. A small focus of abnormal FDG uptake in the lateral basal segment of the left lower lobe corresponds to a small nodule on CT. There are other smaller nodules in the left lung that do not demonstrate abnormal FDG uptake.
Within the right lung, there is a focus of markedly abnormal FDG uptake near the apex that corresponds to soft tissue attenuation about the apical segment right upper lobe bronchus. There is also markedly abnormal FDG uptake about the anterior segment right upper lobe bronchus; this too is associated with soft tissue thickening in a peri-bronchovascular distribution. There is mildly abnormal FDG uptake along the right lower lobe bronchi; this corresponds to thickening seen on the CT. There are other smaller nodules in the right lung that do not demonstrate FDG uptake.
Abnormal radiotracer is noted in several mediastinal lymph nodes. Markedly increased uptake is noted in a lower right paratracheal node as well as a subcarinal node. Uptake around both hila could represent FDG activity in hilar nodes, but it also could represent FDG uptake around the bronchus as described above.
Pneumoconiosis is the general term for lung disease caused by inhalation of mineral dust. Silicosis is a respiratory disease caused by inhalation of silica dust which leads to inflammation and then scarring of the lung tissue.
Silica is a common, naturally occurring crystal. It is found in most rock beds and it forms dusts during mining, quarrying, tunneling, and work with many metal ores. Silica is a principal component of sand, so glass workers and sand-blasters also receive heavy exposure to silica. Risk factors include any work that includes exposure to silica dust. Mining, stone cutting, quarrying, road and building construction, work with abrasives manufacturing, sand blasting and many other occupations and hobbies involve exposure to silica.
Intense exposure to silica may result in disease in a year or less, but it usually takes at least 10 or 15 years of exposure before symptoms develop.
Radiographic studies of the chest are essential to the diagnosis of silicosis. While some chest radiographic findings of silicosis may be nonspecific, others are sufficiently characteristic of the disease. Bilateral alveolar filling and a ground-glass appearance mimicking alveolar proteinosis are observed in silicoproteinosis. Simple silicosis manifests as multiple small (a few mm) nodules that are scattered diffusely throughout the lungs but may be more prominent in the upper lung fields. Calcification of the hilar lymph nodes, particularly in the edge of the nodes (ie, eggshell calcification) is very characteristic of silicosis. However, eggshell calcifications are observed only in a minority of cases of silicosis. Other causes of eggshell calcification include sarcoidosis, histoplasmosis, and irradiation. Rarely, the pulmonary nodules also may show calcification. Complicated silicosis manifests as bilateral upper lobe masses, which are formed by the coalescence of nodules. As these masses retract toward the hilum because of fibrosis, the lower lung fields may appear overinflated.
A CT scan of the chest is more sensitive than chest radiography in discerning the nodules of simple silicosis. In complicated silicosis, a CT scan provides more detail (eg, the presence of cavitation). Although cavitation in silicosis can occur without a mycobacterial infection, such a possibility should be considered when cavitation is observed.
Procedures: Bronchoscopy rarely is needed. The rare indication is in a cavitary or mass lesion when mycobacterial disease or lung cancer is suspected and examination of sputum samples is nondiagnostic.
Histologic Findings: Examination of lung tissue very seldom is necessary because the diagnosis of silicosis is based on history of exposure, symptoms, physical examination findings, and chest radiographic appearance.
The characteristic histopathologic finding is the silicotic nodule mostly located near the respiratory bronchiole. The nodule is composed of refractile particles of silica surrounded by whorled collagen in concentric layers, with macrophages, lymphocytes, and fibroblasts in the periphery. Emphysematous blebs surround the silicotic nodule, especially in the subpleural area. Birefringent crystals of silica in the center of a silicotic nodule may be identified by polarized light microscopy. For definitive identification, scanning electron microscopy combined with x-ray spectroscopy may be needed.
Treatment: There is no specific treatment for silicosis.
Complications: increased risk for tuberculosis, progressive massive fibrosis
References:
1. Varkey B, Varkey AB. Silicosis. eMedicine 2004.
2. MedlinePlus. 2005.
Other Problems to be Considered: Pulmonary tuberculosis, Rheumatoid lung nodules, Metastatic lung cancer
References and General Discussion of PET Tumor Imaging Studies (Anatomic field:Lung, Mediastinum, and Pleura, Category:Inflammation,Infection)
Return to the Teaching File home page.