Case Author(s): Yonglin Pu, M.D.,Ph.D, Farrokh Dehdashti, M.D. , 10/26/2001 . Rating: #D3, #Q4
Diagnosis: Rebound thymic hyperplasia
Brief history:
5-year-old boy with a history of large cell lymphomainitially involving the tonsil, status post resection and chemotherapy, which was completed in July, 2001.
Images:
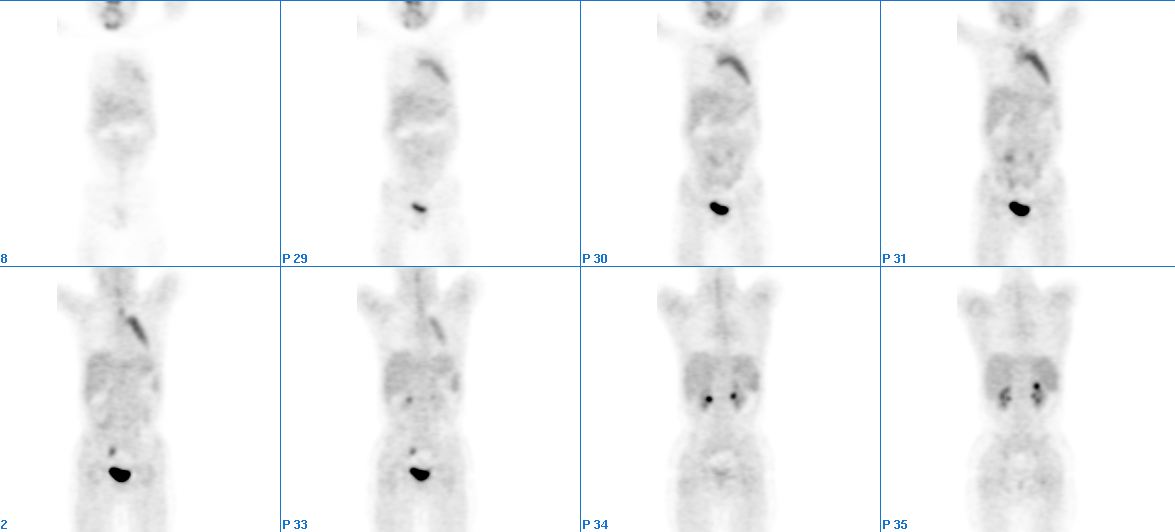
Coronal whole body PET images
View main image(pt) in a separate image viewer
View second image(ct).
Axial chest CT image through the thymus
Full history/Diagnosis is available below
Diagnosis: Rebound thymic hyperplasia
Full history:
5-year-old boy with a history of large cell lymphoma initially involving the tonsil, status post resection and
chemotherapy, which was completed in July, 2001
Findings:
FINDINGS:
TUMOR PET IMAGING (10/26/01):After intravenous administration of F-18 fluorodeoxy-glucose (FDG), a series of overlapping emission and transmission PET images were obtained. The area imaged spanned the region from the neck to the proximal femurs. Diffusely moderately increased uptake is noted in the anterior mediastinum, corresponding to the enlarged thymus demonstrated on the CT study. A small focus of faint abnormally increased uptake is noted within the right axilla, likely inflammation in nature. There are no additional foci of abnormally increased FDG uptake identified.
CT scan of neck, chest, abdomen and pelvis, with oral and nonionic
intravenous contrast(10/23/01): Several lymph nodes within the bilateral posterior jugular chains, measuring less than 5 mm in short axis. When compared to the prior study dated 08/21/01, there has been interval development of a low attenuation soft tissue mass within the anterior mediastinum, just to the left of the aortic arch. This measures 4.0 cm x 3.2 cm in axial dimension.
Discussion:
Most cases of rebound thymic hyperplasia secondary to sucessful chemotherapy (especially in lymphoma or testicular carcinoma) occur within a year and the gland typically returns to normal size (1). Rebound thymic hyperplasia has also been described in patients with endocrine abnormalities such as Graves' disease, acromegaly, and thyrotoxicosis (1). Pathologically, the rebound thymus hyperplasia are composed of the normal proportions of glandular/lymphoid elements in an enlarged gland. The thymus can grow more than 50% after chemotherapy or illness (1).
It is important to differentiate it from residual lymphoma or other tumors on the thymus.
On CT the gland may be normal sized or there may be symmetric enlargement of the gland with preservation of its normal shape and no discrete mass. The borders of the enlarged thymus are most often concave, but occasionally the gland may have a convex margin. Streaks of fat should be identified and the gland should maintain a bilobed appearance (1). There appears to be no specific MRI signal pattern for thymic hyperplasia. (2)
As for PET imaging, if FDG concentration in the thymus reaches the concentration in the bladder or cerebellum, it is suggestive of malignancy (3). Liu et al (4) were able to differentiate between thymus carcinoma and hyperplasia using semiquantitativ eanalysis. However, the number of the patient in the study is too small. Therefore, further studies with large patient population is needed to further evaluate FDG-PET in the differential diagnosis of the two entities.
References:
1. Strollo DC, Rosado-de-Christenson ML Tumors of the thymus. J Thorac Imaging 1999 Jul;14(3):152-71
2. Juhl: Paul and Juhl's Essentials of Radiologic Imaging, 7th ed., Copyright 1998. Lippincott Williams & Wilkins. Page 1125.
3. Brink I, Reinhardt MJ, Hoegerle S, et al. Increased metabolic activity in the thymus gland studied with 18 F-FDG PET. Age dependency and frequency after chemotherapy. J Nucl Med 2001;42(4):591-595
4. Liu RS, Yeh SH, Huang MH, et al. Use of fluorine-18 fluorodeoxyglucose positron emission tomography in the detection of thymoma: a preliminary report. Eur J Nucl Med 1995;22:1402-1407.
Followup:
The patient was on remission for seven months since his last chemotherapy on 02/19/2002. Therefore we think that the enlargement of his thymus on tumor PET imaging was rebound thymic hyperplasia.
Major teaching point(s):
There is no imaging modality that can reliably distinguish thymus rebound hyperplasia from residual/recurrent malignancy. Studies with FDG-PET using small patient population showed that PET is promising in differentiating benign from malignant thymus lesions using a semi- quantitative technique. However further studies are needed to evaluate its usefulness in the differential diagnosis of these conditions in larger group of patients.
Differential Diagnosis List
Residual lymphoma or other tumors on the thymus.
ACR Codes and Keywords:
References and General Discussion of PET Tumor Imaging Studies (Anatomic field:Lung, Mediastinum, and Pleura, Category:Neoplasm, Neoplastic-like condition)
Search for similar cases.
Edit this case
Add comments about this case
Return to the Teaching File home page.
Case number: pt067
Copyright by Wash U MO

