Case Author(s): Gabriel De Simon, M.D. and Jerold Wallis, M.D. , 01/30/01. . Rating: #D2, #Q4
Diagnosis: False negative FDG PET imaging of esophageal cancer.
Brief history:
Several weeks of dysphagia and odynophagia.
Images:
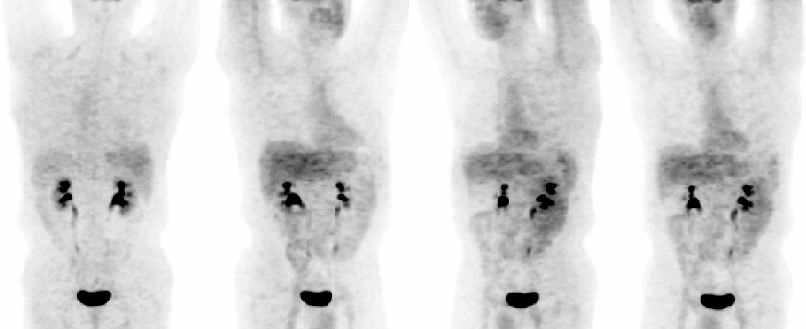
Posterior, RAO, LAO, and Anterior whole body images.
View main image(pt) in a separate image viewer
View second image(pt).
Coronal, transaxial and sagittal whole body images.
View third image(ct).
Transaxial CT images of the lower thorax and upper abdomen.
View fourth image(gs).
Anterior, dual contrast barium image of the stomach.
Full history/Diagnosis is available below
Diagnosis: False negative FDG PET imaging of esophageal cancer.
Full history:
Fifty-five year old male with several weeks dysphagia and odynophagia, in whom an upper gastro-intestinal examination was suggestive of a malignant neoplasm at the gastro-esophageal junction. Subsequent endoscopic examination confirmed the presence of a lower esophageal mass.
Radiopharmaceutical:
14.7 mCi F-18 Fluorodeoxyglucose i.v.
Findings:
FDG PET WHOLE BODY IMAGES:
1. Normal study, with specifically no abnormal FDG uptake in the region of the gastro-esophageal junction where the mass was identified endoscopically.
CONTRAST ENHANCED CT SCAN OF THE CHEST:
1. Soft tissue mass involving the distal esophagus and GE junction.
2. Regional extension of soft tissue with thickening of both diaphragmatic crura, likely related to tumor invasion.
DOUBLE CONTRAST UPPER GI STUDY:
1. Irregularity, lack of normal distension, ulceration and gastric mucosal distortion, consistent with a malignant neoplasm.
Discussion:
FDG PET is of great value and is often used in the detection and staging of gastrointestinal tumors, including esophageal cancers. Although most malignant neoplasms have a higher rate of glucose metabolism compared to normal tissues, there is a wide range in glucose metabolic rate, depending on the aggressiveness and histological subtype of the tumor. Mucinous cancers, which are commonly found in the gastrointestinal tract, typically demonstrate relatively low cell concentrations and have an abundance of intracellular high molecular weight mucin, thereby making FDG PET less sensitive in their detection. In a study by Berger, Nicholson, Dehdashti and Siegel, FGD PET had a lower sensitivity for the detection of primary and recurrent mucinous cancers than generally reported for non-mucin producing tumors. It was demonstrated that failure of PET to reveal tumor foci correlated with the degree of tumor cellularity and abundance of mucin, and that there was no significant correlation between FDG uptake and tumor grade.
In their retrospective review of 22 patients, FDG PET imaging revealed mucinous gastrointestinal cancers in only 13 (59%), an unusually low sensitivity (ie., a high percentage of false negative scans). It is important to understand the potential limitations of FDG PET imaging in patients with mucin-producing tumors.
Reference: Berger K, Nicholson SA, Dehdashti F, Siegel BA. FDG PET evaluation of mucinous neoplasms. AJR April 2000; 174:1005-1008.
Followup:
The patient underwent an esophagectomy with gastric pull-through, and post operative recovery was uneventful. Histological examination of the tumor revealed an invasive, poorly differentiated adenocarcinoma with abundant signet-ring cell types, characterized by intracytoplasmic accumulation of mucin.
Major teaching point(s):
Decreased sensitivity of FDG PET imaging in the detection of gastrointestinal mucin-producing cancers. Understanding of this limitation is essential in PET diagnosis and staging of such tumors.
ACR Codes and Keywords:
References and General Discussion of PET Tumor Imaging Studies (Anatomic field:Gasterointestinal System, Category:Neoplasm, Neoplastic-like condition)
Search for similar cases.
Edit this case
Add comments about this case
Return to the Teaching File home page.
Case number: pt048
Copyright by Wash U MO

