Case Author(s): Stephen Schmitter, M.D. and Tom R. Miller, M.D., Ph.D. , 12/14/00 . Rating: #D3, #Q3
Diagnosis: Recurrent Glioblastoma Multiforme
Brief history:
26 year-old man with a history of glioblastoma multiforme who has undergone resection, chemotherapy and radiation therapy.
Images:
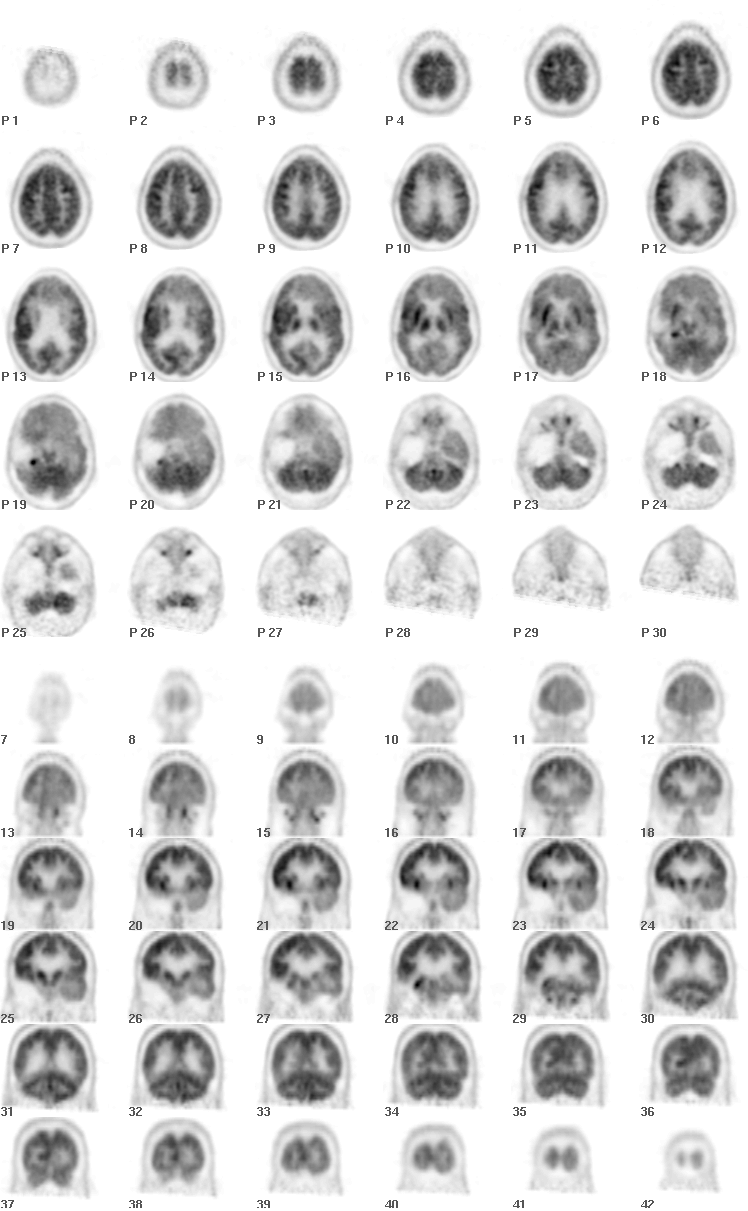
Axial and Coronal FDG-PET Images
View main image(pt) in a separate image viewer
View second image(pt).
FDG-PET Images in the Region of Abnormality
View third image(mr).
Axial T1 Post-Contrast, T2, and Coronal T1 Post-Contrast MRI Images
View fourth image(mr).
MRI and PET Images in a Second Area of Enhancement in the Right Frontal Lobe
Full history/Diagnosis is available below
Diagnosis: Recurrent Glioblastoma Multiforme
Full history:
26 year-old man with a history of a right temporal glioblastoma multiforme who has undergone resection, chemotherapy and radiotherapy. Resection was repeated 5 months later for recurrent glioblastoma. He presents approximately 4 months after the second resection with weakness, worsened coordination,and difficulty with speech, memory and mentation.
Radiopharmaceutical:
10.0 mCi F-18 Fluorodeoxyglucose i.v.
Findings:
Axial and coronal PET images demonstrate post-operative changes from partial right temporal lobe resection. Focal hypermetabolism is present at the posteromedial aspect of the surgical bed. This area is better seen in the second set of images.
Corresponding MRI images also demonstrate post-surgical changes and focal enhancement at the posteromedial aspect of the surgical bed (third image).
A second area of enhancement is present anterolateral to the right frontal horn. Decreased metabolism is seen in this region on PET images (fourth image).
Discussion:
Differentiating recurrent glioblastoma multiforme from post-radiation changes is often very difficult. The clinical and imaging features of these entities can be identical. Radiation injury can be divided into acute (hours to weeks), early delayed (weeks to 4 months) and late delayed (4 months to years). Late delayed radiation injury (LDRI) is due to vascular endothelial injury or direct damage to oligodendroglia. It is this stage of injury that is most likely to be confused with recurrent tumor. Both tumor and LDRI can present on CT or MRI as a contrast-enhancing mass with edema and mass effect. The rationale behind using FDG-PET in this setting is the fact that areas of radiation injury have lower glucose metabolism than tumor or normal brain tissue because they are less cellular. Studies have reported sensitivity and specificity of FDG-PET in differentiating tumor from LDRI of 81-86% and 40-94%, respectively.
In this case, increased metabolism was seen in the region of enhancement at the posteromedial aspect of the surgical bed, consistent with recurrent tumor. Decreased metabolism was seen in the focus of enhancement adjacent to the right lateral ventricle, consistent with LDRI.
Increased uptake can sometimes also be seen during normal healing processes during the first several months following radiation or surgery. Other potential causes of false positive studies are abscesses and seizure foci.
Reference:
Langleben, DD, and Segall, GM. PET in Differentiation of Recurrent Brain Tumor from Radiation Injury. J Nucl Med. 2000;41:1861-1867.
Followup:
Some of the patient's new symptoms were attributed to an acute right cerebellar infarct noted on diffusion-weighted images (not shown). The remainder of his decline was felt to be secondary to a combination of recurrent tumor and radiation injury. Because of his poor prognosis and second recurrence, he was not felt to be a surgical candidate. Chemotherapy was continued and he was transferred to a nursing home.
ACR Codes and Keywords:
References and General Discussion of PET Tumor Imaging Studies (Anatomic field:Skull and Contents, Category:Neoplasm, Neoplastic-like condition)
Search for similar cases.
Edit this case
Add comments about this case
Return to the Teaching File home page.
Case number: pt043
Copyright by Wash U MO

