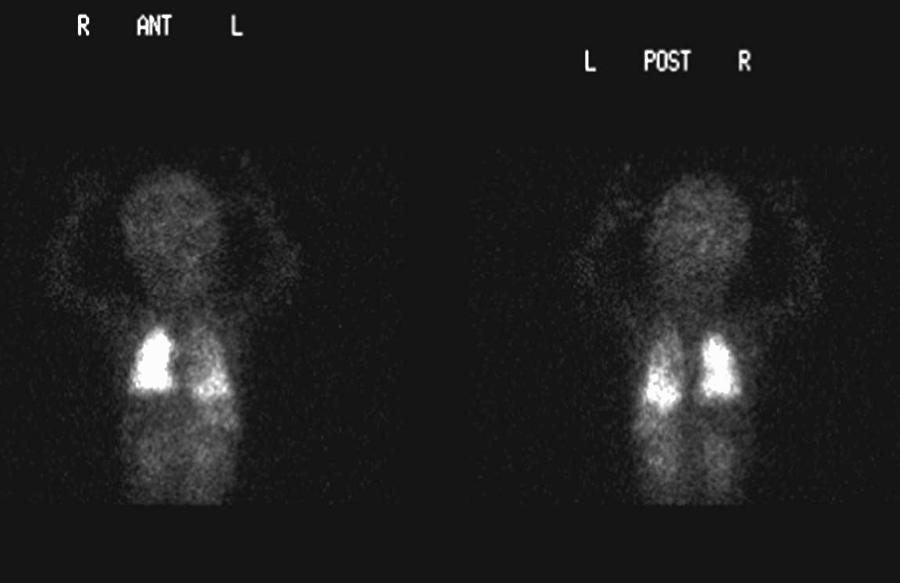

Images of pulmanary perfusion scintigraphy
View main image(pe) in a separate image viewer
View second image(pe). Pulmanary perfusion scintigraphy - spot views
View third image(xr). Chest radiograph
View fourth image(pe). Quntitative activity of whole body and lungs (lower data are lungs vs the rest of the imaged body)
Full history/Diagnosis is available below
The perfusion images show diffusely decreased activity in the left lung, with slightly more prominent activity in the left lung base.
The right lung receives 65% and the left lung receives 35% of total pulmonary perfusion.
Analysis of the global pulmonary activity as compared to the systemic activity demonstrates approximately 60% of activity in the lung and approximately 40% in the remainder of the visualized portions of the body. The findings are consistent with a marked right-to-left shunt.
The presence of extrapulmonary activity on perfusion scintigraphy indicates the presence of free Tc-99m pertechnetate or an intra- or extracardiac right-to-left shunt. In a right-to-left shunt, the radiopharmaceutical will accumulate in the systemic capillary beds, primarily the kidneys, brain, and spleen. In contrast, free Tc-99m pertechnate will accumulate most prominently in the stomach, thyroid, salivary glands, and kidneys. An image of the head is the most definitive way to distinguish between a right-to-left shunt and free Tc-99m pertechnetate because intracerebral activity is present with a shunt but not when there is free Tc-99m pertechnetate.
Normal patients should have more than 90% of radioactivity in the lungs. Pulmonary accumulation of Tc-99m MAA drops as a function of time and become less than 90% after 30 min because of breakdown of the MAA. Timing is thus importnat in evaluating a shunt.
Absolute quantification, including the pulmonary to systemic perfusion ratio (Qp/Qs) is possible, but was not completely done in the case because the entire body was not imaged.
References:
1. Hosono M, Machida K, Honda N. Quantitative lung perfusion scintigraphy and detection of intrapulmonary shunt in liver cirrhosis. Annals of Nuclear Medicine. 2002; Vol. 16, No. 8, 577–581.
2. Gang L, Wei-jen S, Chou C, et a. Tc-99m MAA Total-Body Imaging to Detect Intrapulmonary Right-to-Left Shunts and to Evaluate the Therapeutic Effect in Pulmonary Arteriovenous Shunts. Clinical Nuclear Medicine. 1996; 21(3):197-202.
3. Verttukattil JJ, et al. Radionuclide investigation of congenital heart disease. Heart 2000;84:467-468.
4. MIR Teaching file case vq026.
5. Ziessman HA, Rehm P. Case review: nuclear medicine. Mosby, Inc. 2002.
References and General Discussion of Perfusion (only) Scintigraphy (Anatomic field:Lung, Mediastinum, and Pleura, Category:Normal, Technique, Congenital Anomaly)
Return to the Teaching File home page.