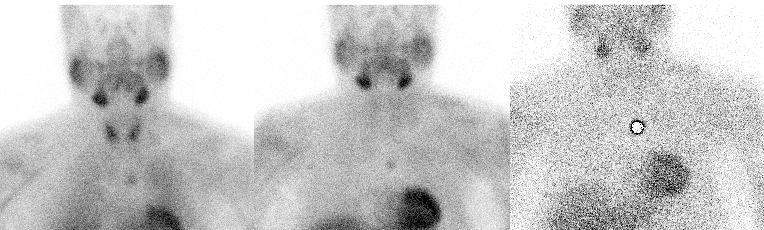

Anterior images (10-minute, 2-hour and 2-hour with a radioactive marker)
View main image(pa) in a separate image viewer
View second image(pa). SPECT axial, coronal and sagittal images.
View third image(ct). Computed Tomography image of the upper mediastinum.
Full history/Diagnosis is available below
The upper parathyroid glands arise with the lateral anlages of the thyroid from the fourth branchial pouch and maintain a fairly constant final position (usually behind the middle third of the thyroid). The lower parathyroid glands arise with the thymus from the third branchial pouch and descend to their final position. They are usually located lateral to the lower poles of the thyroid, but have a large degree of variability, ranging from the angle of the mandible to the lower anterior mediastinum.
Primary hyperparathyroidism occurs in 1 of 700 adults and is due to parathyroid adenoma in 80 to 85% of cases, parathyroid hyperplasia in 10 to 15%, multiple parathyroid adenomas in 2 to 3% and parathyroid carcinoma in less than 1%. Clinical features include bone pain, renal calculi and occasional psychiatric disturbances. Secondary hyperparathyroidism occurs in chronic renal failure in which calcium metabolism is altered leading to enlargement of the parathyroid glands. Tertiary hyperparathryroidism results from secondary hyperparathyroidism when chronically overstimulated parathyroid glands begin to secrete autonomously.
In the hands of an experienced surgeon, a parathyroid adenoma can be resected without the aid of prior imaging in the majority of cases (greater than 90%). Imaging can nonetheless be helpful to enable limited surgery, increase success rates further, and to locate ectopic glands. When hyperparathyroidism persists after an initial surgical attempt is made to remove an adenoma, imaging is indicated to locate a possible ectopic gland.
Scintigraphy is limited due to lack of a radiopharmaceutical that is exclusively taken up by parathyroid tissue. Se-75-selenomethionine was an early parathyroid imaging agent. During protein synthesis, it was incorporated as an analog of methionine. However, it was not a sensitive or specific imaging technique. More successful scintigraphic techniques to localize parathyroid adenomas have included subtraction techniques between Thallium-201 (taken up by both thyroid and parathyroid) and Tc-99m pertechnetate (taken up by thyroid but not parathyroid), or between Tc-99m sestamibi and I-123 or Tc-99m pertechnetate. Imaging with Tc-99m sestamibi alone, utilizing the higher uptake and slower washout of sestamibi from the parathyroids relative to the thyroid, has been shown to have a higher sensitivity and accuracy than the Tl-201/pertechnetate subtraction technique.
Sensitivity may be increased slightly (with substantial increased tracer cost) by administering I-123 in addition to the Tc-99m sestamibi and obtaining a simultaneous, dual-energy acquisition. A subtraction image (I-123 image subtracted from the sestamibi image) may be obtained. Alternatively, a simple comparison of the two images may reveal a contour change consistent with a parathyroid adenoma.
In sestamibi dual-phase parathyroid imaging, the patient is injected with 10-20 mCi of Tc-99m sestamibi. Anterior early static images at about 10 minutes and delayed static images at 1 1/2 to 3 hours are obtained. A persistent focus of activity relative to the thyroid gland is consistent with a parathyroid adenoma. SPECT imaging is often helpful to better localize the adenoma. If SPECT imaging is to be performed, it is best done early so that sufficient activity remains in surrounding structures to yield anatomic localizing information. If a skin site is to be marked for the surgeon, the patient should first extend the neck in the same manner as it would be during surgery. In some cases, the surgeon may elect to use an intraoperative gamma probe to help localize a parathyroid adenoma, immediately following sestamibi parathyroid imaging. Since the target-to-background ratio is not as good as it is for sentinel node localization following intradermal lymphoscintigraphy, the use of an intraoperative gamma probes is more difficult.
References:
Loevner, Laurie. Imaging of the Parathyroid Glands. Sem in Ultrasound, CT, and MRI. Vol 17: No 6; Dec, 1996, pp 563-575.
Shaha A., Sarkar S., Strashun A and Yeh, S. Sestamibi scan for preoperative localization in primary hyperparathyroidism. Head & Neck; Mar, 1997, pp 87-91.
Martinez D, et al. Intraoperative identification of parathyroid gland pathology: a new approach. J of Ped Surg. Vol 30: No 9; Sep, 1995, pp 1306-1309.
Petti, George. Hyperparathyroidism. Otolar Clin N Am. Vol 23; No 2, 1990, pp 339-355.
Price, David. Radioisotopic evaluation of the thyroid and the parathyroids. Endocrine radiology. Vol 31: No 5; Sep 1993, pp: 991-1015.
References and General Discussion of Parathyroid Scintigraphy (Anatomic field:Lung, Mediastinum, and Pleura, Category:Metabolic, endocrine, toxic)
Return to the Teaching File home page.