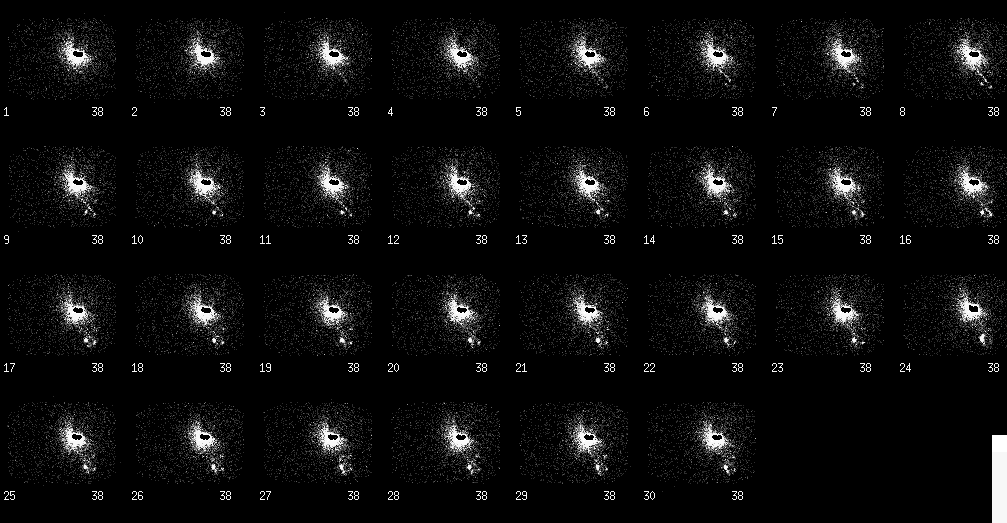

Anterior dynamic flow images.
View main image(lm) in a separate image viewer
View second image(lm). Spot emission and transmission images.
Full history/Diagnosis is available below
In cutaneous malignancies such as melanoma, drainage can be variable. For example, a site on the shoulder could drain to lymph nodes in the neck, the supraclavicular region, the axilla, or the mediastinum. Thus, it is important to define the nodes draining the area of interest. The first set of nodes that drain the area of interest are called the "sentinel nodes."
Performing this study within 1-2 weeks of an excisional biopsy may decrease the sensitivity for detecting the normal lymphatic drainage to the sentinel nodes. The presumed mechanism for this adverse effect is "clogging" of the lymphatic channels and lymph nodes by the debris cre- ated by the excisional biopsy. It is not clear, based on published data, whether this is an important practical issue.
The lymphatic draininage of a cutaneous lesion can be mapped by injecting millipore-filtered sulfur colloid intradermally around the lesion. Injecting directly into the lesion is not recommended as the lymphatic channels may be disrupted by the growth of the malignancy. The sulfur colloid will be collected and drained by the lymphatics and subsequently phagocytosed by macrophages within the sentinal lymph nodes. Typically, a 60-frame (30 seconds per frame) dynamic study is obtained for 30 minutes followed by static images obtained 2-3 hours post-injection. Foci of increased radiotracer accumulation do not necessarily represent lymph nodes involved by malignant disease as the tracer is not specific for malignant cells. Rather, the tracer identifies the first lymph nodes that filter the lymphatic drainage from an area of interest.
A transmission scan can be performed to assist in anatomically localizing the sentinel nodes. A brief (10 -econd) transmission image with a Co-5) flood source positioned behind the patient will outline the contour of the body. Alternatively, a small syringe of Tc-99m pertechnetate could be used as a marker to "trace" an outline of the body contour. Further localization is performed via surface marking and, depending on the surgeon, via a gamma probe during surgery. Once these nodes are located, they can be excised and examined for histologic or immunohistochemical evidence of metastatic disease.
2) Lymphoscintigraphy maps lympatic drainage, not tumor spread
3) A transmission image helps provide anatomic landmarks for localization
4) Lymphoscintigraphy can help localize nodes during surgery
References and General Discussion of Lymphoscintigraphy (Anatomic field:Vascular and Lymphatic Systems, Category:Neoplasm, Neoplastic-like condition)
Return to the Teaching File home page.