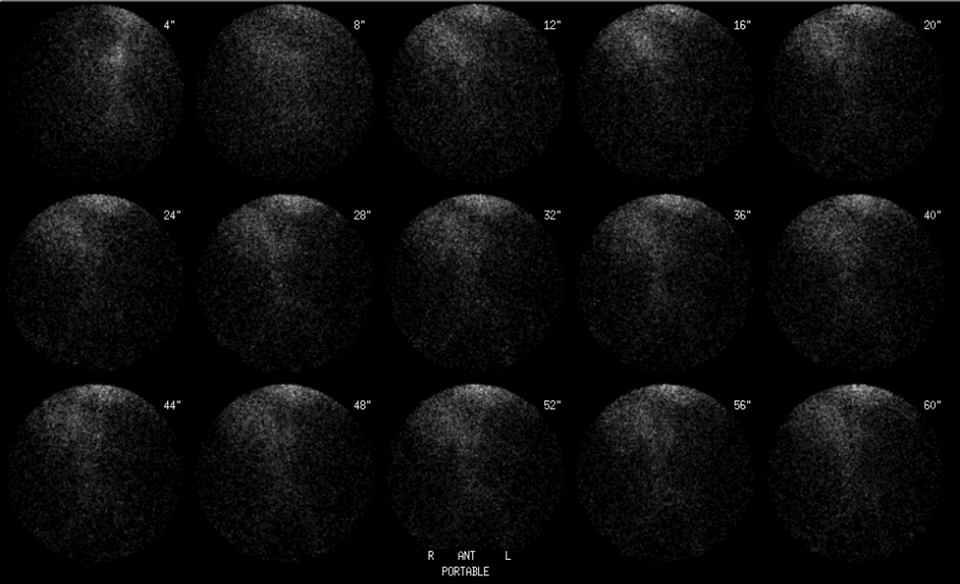

Anterior radionuclide angiogram
View main image(gi) in a separate image viewer
View second image(gi). Serial 5 minute anterior static images (initial)
View third image(gi). Serial 5 minute anterior static images (delayed)
Full history/Diagnosis is available below
View followup image(an). Visceral angiogram with sub-selective injection of the right colic artery.
The most common cause for occult GI bleeding is upper GI bleeding. Since scintigraphy is not helpful for management of upper GI bleeding, an upper endoscopy, or at the very least a NGT aspirate should be performed in patients when UGI bleeding is a the possible cause for GI bleeding.
In order for a radionuclide GI bleeding study to be positive, the patient must have significant bleeding (50-100 mLs) over the period of imaging (generally 90 minutes). Reliable signs of significant active bleeding include orthostatic hypotension, an increase in resting pulse rate and a decrease in urine output. Passing bright red blood per rectum is a less reliable sign since the colon serves as a resevoir for the blood and there is not necessarily a good correlation between active bleeding and colon evacuation. The purpose of nuclear medicine is not to diagnose or confirm bleeding - this is already known. The purpose is to determine if the patient has significant enough active bleeding that arteriography is likely to be positive. In addition, the radionuclide GI bleeding study can often localize the bleeding source thus facilatating surgical, endoscopic or interventional radiology treatments.
Knowledge of the arterial supply of the colon and rectum is essential in directing the interventional radiologist and surgeon.
Activity within loops of bowel move over time due to peristalsis, and can move in both directions; therefore it is essential to acquire images continuously in order to identify the point where bleeding first appears on the scan. A cine-mode display so you can review individual frames is also critical. Temporal resolution of at least 1 frame per minute is recommended.
Rectal bleeding can be obscured by overlying bladder activity. A posterior view and imaging the bedpan contents (if any have been passed after the injection of radiopharmaceutical) may be required to make this diagnosis.
The presentation and patterns of bleeding for the above entities are widely varied, and for this case, many are not applicable.
For this specific case, with known diverticulosis, the first entity is the most likely diagnosis.
References and General Discussion of Gastrointestinal Bleeding Scintigraphy (Anatomic field:Gasterointestinal System, Category:Organ specific)
Return to the Teaching File home page.