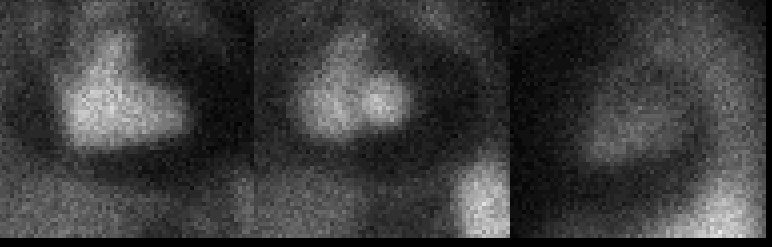

Anterior, Best septal, and Lateral images from a cardiac blood pool study.
View cine in AVI format.
View main image(ca) in a separate image viewer
View second image(xr). Top images: Frontal and lateral views from a chest radiograph. Obtained on the same day as the Tc-99m-RBC cardiac blood pool examination. Bottom Image: Static end-diastolic (ED) and end-systolic (ES) images from the Tc-99m-RBC cardiac blood pool examination.
Full history/Diagnosis is available below
Chest radiograph: There is thickening of the right paratracheal stripe and tracheal deviation consistent with lymphadenoapathy. Cardiac silhouette enlargement (water bottle configuration) is compatible with the large pericardial effusion.
When pericardial effusions develop, cardiac chamber capacity may be reduced. Because venous return may be impaired, cardiac output would be limited. Slow accumulation of large amounts of fluid may collect without producing clinical symptoms. On the other hand, rapid accumulation of fluid is tolerated poorly with nonspecific symptoms of dyspnea, chest or shoulder pain, or orthopnea. Physical examination demonstrates a paradoxical pulse, jugular venous distension, faint heart sounds, and a friction rub. EKG changes are nonspecific but include low voltage QRS complexes, ST segment elevation, T wave inversion and development of arrhythmias. Electrical alternans, (beat-to-beat) variation in QRS amplitude, occurs with excessive motion of the heart within the fluid-filled pericardial space.
In cardiac blood pool or cardiac perfusion imaging examinations, absence of tracer activity around the cardiac chambers or myocardium, respectively, is due to a pericardial effusion that may be comprised of serous fluid, hemorrhagic fluid, purulent debris, or chylous fluid (or a combination).
On echocardiography, pericardial effusions are characterized by sonolucency between the visceral and parietal pericardium.
Treatment of a pericardial effusion involves correcting the underlying cause. Pericardiocentesis may be performed in patients with impending tamponade. Pericardiotomy may be performed if effusions recur. Rarely pericardial sclerosis may be performed on recurrent effusions using sclerosing agents such as tetracycline or doxycycline.
REFERENCES:
Strimel WJ and Noe S. (2002, October 9). Pericardial Effusion. eMedicine. Retrieved November 29, 2003, from http://www.emedicine.com/med/topic1786.htm.
Venugopalan, P. (2003, July 1). Pericardial Effusion, Malignant. eMedicine. Retrieved November 29, 2003, from http://www.emedicine.com/ped/topic1764.htm.
Sprengelmeyer JT et al. (1990), Journal of Nuclear Medicine. “Phosphorous 32 colloidal chromic phosphate: treatment of choice for malignant pericardial effusion.” 31:2034-6.
View followup image(ct). Images from CT chest examination (obtained 6 weeks prior to the cardiac blood pool examination) demonstrate a large infiltrative mass with central necrosis in the anterior mediastinum. Mediastinal lymphadenopathy extends to the right hilum. Right axillary, paratracheal, bilateral supraclavicular and hilar lymphadenopathy are also demonstrated. CT of the neck, abdomen and pelvis (images not shown) revealed extensive cervical lymphadenopathy. No abdominal lymphadenopathy or splenomegaly is appreciated.
References and General Discussion of Cardiac Blood Pool Scintigraphy (Anatomic field:Heart and Great Vessels, Category:Organ specific)
Return to the Teaching File home page.