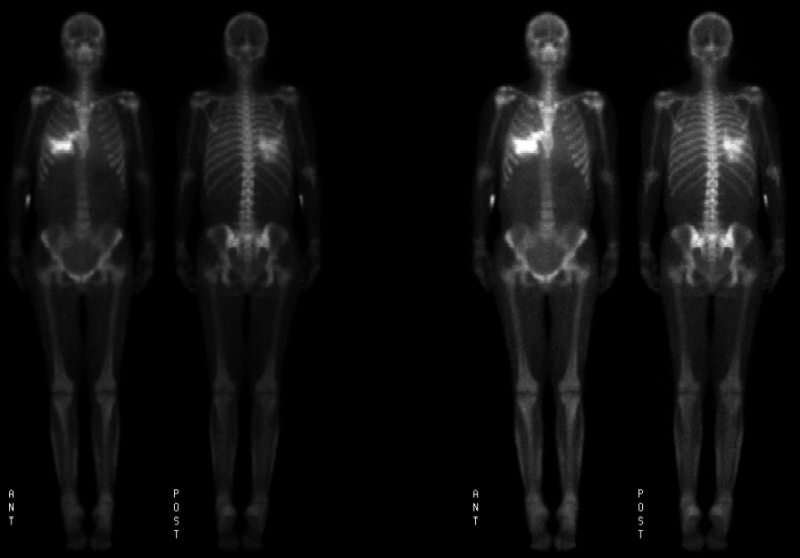

Anterior and posterior images are shown
View main image(bs) in a separate image viewer
View second image(bs). Spot images (left) and coronal (above) and axial (below) SPECT images are shown
View third image(xr). Plain radiographs
View fourth image(ct). Chest radiograph and computed tomography images
Full history/Diagnosis is available below
Current labs include: Calcium 10.6 (high); Ionized calcium 5.28 (high); Phosphorus 9.0 (very high); PTH, intact <5 (low) (? nonfunctioning implant); Calcium-Phosphorus product 90 (high).
Tibia/Fibula radiograph shows subtle soft-tissue swelling with superimposed fine reticular calcification, also consistent with calciphylaxis.
Chest radiograph shows bibasilar infiltrates and effusions.
Computed tomography confirms the right middle lobe and left lower lobe infiltrates and effusions. The CT also shows calcification in the right middle lobe, correlating with the uptake on bone scan.
The incidence is up to 4% per year in peritoneal dialysis patients, and it is also seen in post-transplant patients. Increasing freqency may be due to use of calcium and vitamin D supplments in these patients. Risk factors include a high calcium-phosphorus product (>70), female sex, peritoneal dialysis, diabetes, hyperparathyroidism, and oral CaCO3 dose.
The bone scan is the test of choice and can be positive in up to 97% of patients, usually demonstrating subcutaneous uptake in areas of plaques. If deep ulcerations are present, there can be loss of subcutaneous calcium containing tissue, and the bone scan will be negative. Conventional radiographs can be negative in 29%; when positive they can range from a subtle, diffuse, fine reticular pattern of calcification to a very coarse reticulo-nodular calcification.
Treatments have included oral prednisone for 3-8 wks, which showed 80% improvement in one study with a ~20% relapse rate in 2-6 months. Parathyroidectomy has been helpful in patients with PTH greater than 4 times normal, after which all cases improved or were cured in one study. Parathyroidectomy may not help patients who already have ulcers. Use of non-calcium containing phosphate binders is useful for prevention. Hyperbaric oxygen is of possible help in trying to reverse ulceration.
Outcome is generally poor, with mortality in patients only with plaques approximately 40% by one year in one study. Mortality with ulcers was reported at 67% by one year in the same study. However, if a patient developed ulcers from plaques, mortality was 89% by one year. Biopsy of the lesions can be dangerous as it can cause non-ulcerating plaques to ulcerate and result in rapid progression of disease and death. Related causes of death included sepsis, weight loss/malnutrition (from analgesics), stopping dialysis. Most patients also have multiple co-morbid conditions which could contribute to mortality.
Reference: Fine and Zacharias, “Calciphylaxis is usually no-ulcerating: Risk factors, outcome and therapy,” Kidney International, Vol 61 (2002), pp. 2210-2217.
References and General Discussion of Bone Scintigraphy (Anatomic field:Vascular and Lymphatic Systems, Category:Metabolic, endocrine, toxic)
Return to the Teaching File home page.