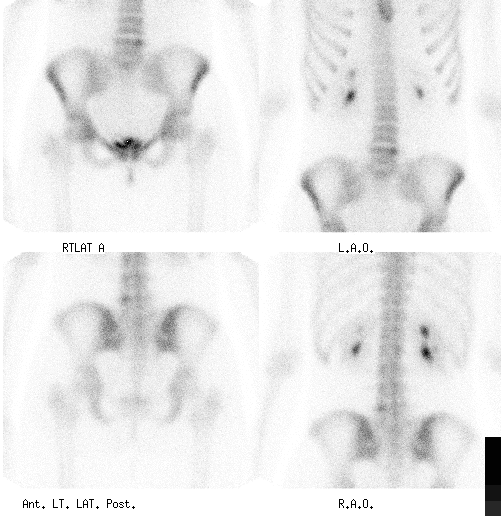

Anterior and posterior spot images of the pelvis and lumbar spine.
View main image(bs) in a separate image viewer
View second image(mm). Axial, coronal and sagittal SPECT images of the lumbar spine
View third image(xr). Oblique plain radiographs of the lumbar spine.
Full history/Diagnosis is available below
Plain Radiographs were obtained including oblique and coned examination of the lower lumbar spine. There was no radiographic evidence of a pars interarticularis defect. Instead, there is a lytic lesion involving the inferior aspect of the left L5 pedicle best seen on the oblique view. Differential diagnosis includes benign primary bone tumors including osteoblastoma or osteoid osteoma. Less likely etiologies would include an aneurysmal bone cyst or giant cell tumor.
Osteoid osteoma is the most common benign tumor of the spine. Patients are young and commonly present with pain and occasionally scoliosis with apex away from side of the lesion. All three stages of the triple phase bone scan are abnormal showing initially increased blood flow and increased radiopharmaceutical deposition on the later images at the site of the lesion. Classically, there is a “hot” nidus related to hypervascularity in the center of the lesion and a less intense peripheral zone related to the rim of bone sclerosis. Osteoblastomas, are larger (> 1.5 cm) than osteoid osteomas, are commonly less painful and have a natural history of progressive growth rather than spontaneous remission.
Treatment options of osteoid osteomas are limited. Non-steroidal anti-inflammatory medications are the most commonly used option. Radiofrequency (RF) ablation has been used successfully on these lesions and involves introduction of a metallic probe into the center of lesion under CT-guidance and ablation of the by controlled increase in the temperature around the tip of the probe.
References:
Textbook of Nuclear Medicine ed. Michael A. Wilson, Lippincott-Raven Publishers 1998
Clinical Nuclear Medicine Ed. MN Maisey, KE Britton, BD Collier Chapman and Hall Medical 3rd edition 1998
References and General Discussion of Bone Scintigraphy (Anatomic field:Spine and Contents, Category:Neoplasm, Neoplastic-like condition)
Return to the Teaching File home page.