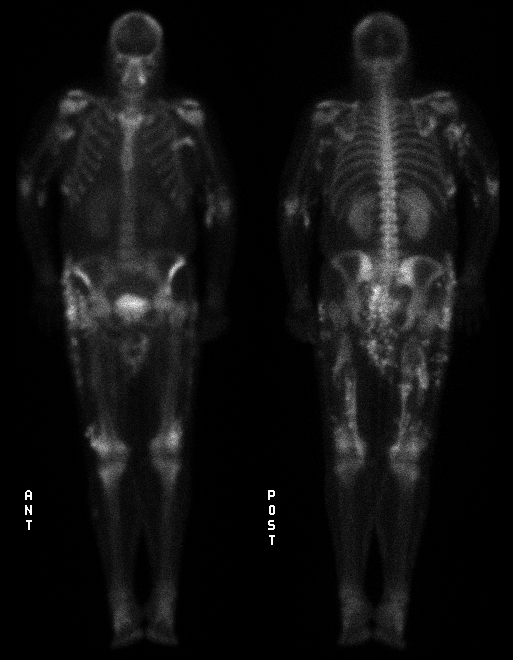

Anterior and posterior whole body scintigrams
View main image(bs) in a separate image viewer
Full history/Diagnosis is available below
Renal enlargement is likely secondary to acute glomerulonephritits
The pathophysiology of calcinosis cutis is unclear. Local elevations in alkaline- phosphatase activity may prevent pyrophosphate inhibition of calcium deposition. Another proposed mechanism is nidus formation produced by phosphate binding to DNA proteins of necrotic cells at sites of inflammation or trauma. Lastly,local tissue injury may produce increased cell membrane permeability allowing influx of calcium, which exceeds the mitochondrial capacity to sequester the mineral. Subsequently, the mitochondria release this calcium phosphate to matrix vesicles which have been proposed as the site of initial extracellular calcium deposition.
Therapy of calcinosis is primarily medical. Intralesional injections of steroids is occasionally effective. Etidronate disodium, a diphosphonate, has been used to inhibit biomineralization. Excessive dosages have led to fractures and osteomalacia, however. Alumina hydroxide ,an oral phosphate binding agent ,has been useful in some cases of calcinosis due to dermatomyositis. Surgical therapy for symptomatic relief of calcinosis cutis has also been proposed but the effectiveness of this therapy remains to be proven.
References: 1) Cuzins, et al. Surgical management of calcinosis cutis universalis and systemic lupus erythematosus. (In press).
2) Rothe, et al. Extensive calcinosis cutis with systemic lupus erythematosus. Arch of Derm 126(8): 1060-1063, 1990.
3) Weinberger, et al. Extensive soft tissue calcification (calcification universalis) in systemic lupus erythematosus. Ann Rheum Dis 38:384-386, 1979.
References and General Discussion of Bone Scintigraphy (Anatomic field:Skeletal System, Category:Metabolic, endocrine, toxic)
Return to the Teaching File home page.